Glaucoma

Glaucoma is defined as various pathological entities. Common point of all is the at an advanced stage destruction of the optic nerve head on the background of the eye globe (optic disc). The causes as well as the disturbances may be different each time, but the common element is always the destruction over time of nerve fibers.
Normal Optic Disc
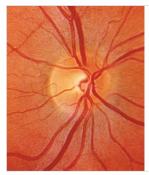
Glaucoma Optic Disc
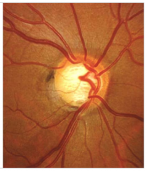
How does the glaucoma occur?
In the eye there is the so-called anterior (between the cornea and the iris) and the posterior (between iris and lens) chamber. These two chambers are full of aqueous fluid produced by the epithelium of the radial body and through the pupil reaches the anterior chamber.
Types of glaucoma :
Primary open-angle glaucoma: caused by a disturbance of the balance between intraocular pressure and blood flow of the optic nerve. It can also occur in statistically “normal” eye pressure conditions.
Primary angle blocking glaucoma or closed-angle glaucoma due to narrowing of the front chamber angle.
Primary congenital glaucoma in newborns and children due to poor tissue maturation.
Secondary glaucoma due to increased pressure because of or as complication of other eye diseases (inflammations, injuries, diabetes mellitus and other vascular eye diseases) in the course of which inhibition of the outflow of aqueous fluid is caused.
Who is affected by glaucoma?
About 4% of all people are affected during their lifetime by glaucoma, usually after the age of 40. Risk factors are:
Παράγοντες κινδύνου αποτελούν:
- Age over 65
- History of inheritance
- Cardiovascular diseases
- Severe intraocular inflammations
- High myopia / hyperopia
- Cortisone therapy
- Nicotine
Annoyances, symptoms?
- Primary open-angle glaucoma is the most common form. It starts unnoticed without causing pain. Incurable causes damage to the optic nerve with deficits in the field of vision and ultimately blindness.
- In closed-angle acute glaucoma, strong pains in the eye and head appear, a sharp decrease in vision, often a tendency to vomit or vomit. The eyeball is reddish and hard
- Newborns suffering from congenital glaucoma show unusually “beautiful – large” eyes, photosensitivity and tearing.
Diagnosis of glaucoma.
Diagnosis is made with the help of clinical and paraclinical examinations. The optic nerve can be examined by the glaucoma-experienced ophthalmologist in the spalt lamp. A modern method is the three-dimensional representation of the optical disc and calculation of the thickness of the nerve fiber layer of the retina through the emission of a LASER beam in the context of an OCT examination.
With the help of an eye tonometer, intraocular pressure can be measured. This is normally below 21 mmHg, on average at 15 mmHg. Alternatively, the pressure can be measured with the air tonometer without instilling a drop and contact of a tool with the cornea, but the measurement is often not so reliable.
In addition, an examination of the central visual field, the so-called automatic perimeter, is carried out to identify any existing deficits of visual field. It is noted that the patient may suffer from glaucoma even if he has normal intraocular pressure (primary open-angle glaucoma with normal pressure) or normal field of vision (preperimetric glaucoma). It has been found that even after the destruction of 45% of the nerve fibers of the retina, the result of the examination of the visual field may be perfectly normal.
To discover and treat glaucoma in a timely manner before they appear severe, irreversible lesions are recommended after the age of 40 years of annual preventive control.


Therapy
The aim of treatment is mainly to reduce intraocular pressure in order to stabilize the condition and avoid further damage to the optic nerve.
The acute glaucoma requires immediate, urgent treatment because incurable can lead within a few hours to blindness. Treatment is both conservative (instillation of collars, intravenous administration of drugs that drastically reduce intraocular pressure) and surgical (iridotomy with YAG-Laser, iridectomy).
Congenital glaucoma in newborns should be treated surgically as quickly as possible.
In chronic open-angle glaucoma, the most common form in adult, the treatment is aiming to reduce the eye pressure with daily use of antiglaucoma drops. Some of the antiglaucomas reduce the production of aqueous fluid, others improve its outflow. The type and frequency of taking these medicines is adjusted each time depending on the patient. Most of the time, medication is sufficient in terms of regulating pressure.
If the medication proves inadequate as well as in case of side effects or intolerance, surgical treatment is considered. The methods followed are as follows:
Outflow of aqueous fluid from the anterior chamber under the conjunctiva through the construction of an “artificial pathway” of outflow to open-angle glaucoma (trabeculectomy, deep sclerotomy).
Deepening of the anterior chamber by removing a part of the iris (YAG-Laser, iridectomy) or by cataract surgery.
Installation of a drainage valve of the aqueous fluid from the anterior chamber under the conjunctiva.
Laser trabeculoplasty in open-angle glaucoma.
Ahmed valve

Prognosis:
Incurable glaucoma leads in the long run to blindness. Early diagnosis and proper treatment are crucial because the lesions of the optic nerve are irreversible. With the right treatment the goal is most often achievable and the progression of the disease is interrupted.
Glaucoma is often hereditary. In case of affection of a relative, an eye check must be carried out no later than the age of 35.
Types of glaucoma
Primary glaucoma
Primary glaucomas are those whose cause is not another eye disease.
Open angle glaucoma
It is the most common form of glaucoma. It usually occurs after the age of 30 but can appear earlier. Heredity is common.
“Normal pressure” glaucoma
It belongs to the category of primary glaucoma. Characteristic is the damage of the optic nerve despite normal pressure. Patients in this category experience limited blood flow of the optic nerve and sometimes sleep apnea as well as low blood pressure mainly during night sleep as well as feeling of numbness of the extremities.
Congenital glaucoma
Through a disturbance of the growth of the angle of the front chamber during the embryonic period, difficulty of outflow of the aqueous fluid occurs. It may coexist with other physical deformities. High intraocular pressure can cause a one-sided or bilateral increase in the size of the eyeball (buphthalmos, hydrophthalmos). In case of suspected congenital glaucoma it is necessary to immediately examine and measure the intraocular pressure in total anesthesia and if surgical treatment is deemed necessary in order to avoid permanent damage.
Acute closed-angle glaucoma
Closed-angle acute glaucoma suddenly appears due to inhibition of the outflow of aqueous fluid from direct contact of the anterior surface of the lens with the posterior of the iris which causes obstruction of the angle of the anterior chamber. The sharp increase in pressure to levels even above 60 mmHg causes sudden loss of vision, strong pains in the eye and head, tearing, propensity for vomiting and vomiting; almost always only one eye is affected; this acute glaucoma crisis may subside and re-occur in the future.
Chronic closed-angle glaucoma
The increase in pressure is also caused by partial obstruction of the anterior chamber angle. High hyperopia and advanced cataracts are the main risk factors. Systematic administration of drugs and instillation of drops in order to reduce intraocular pressure as well as contraction of the iris (muscle), iridotomy with YAG-Laser, surgical iridectomy and cataract surgery are the therapeutic options of this type of glaucoma.
Secondary glaucoma
Glaucoma caused by eye diseases or generalized diseases is called secondary. The most common causes are pseudoexfoliation syndrome, proliferative retinopathy due to diabetes mellitus, retinal vein or artery occlusion, intraocular inflammation (uveitis), eye tumors, topical or systemic steroid therapy, trauma and pigment dispersion syndrome.

