Retinal vascular occlusion

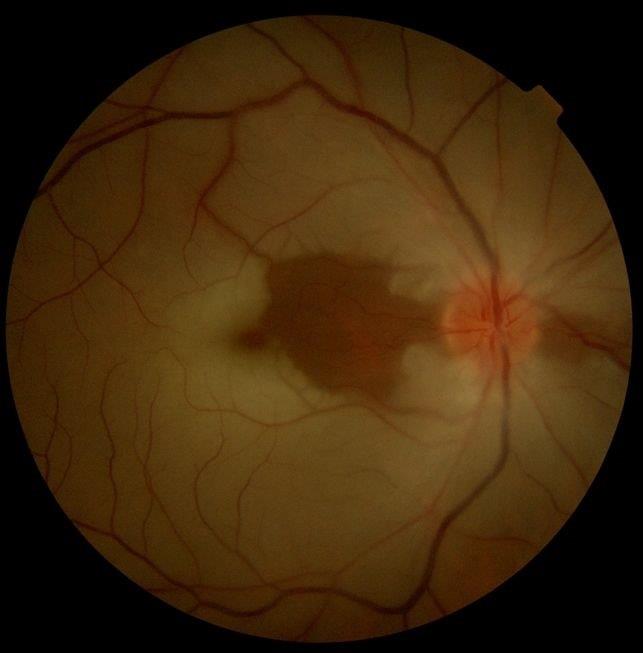
Retinal Artery Occlusion
Central Retinal Vein Occlusion
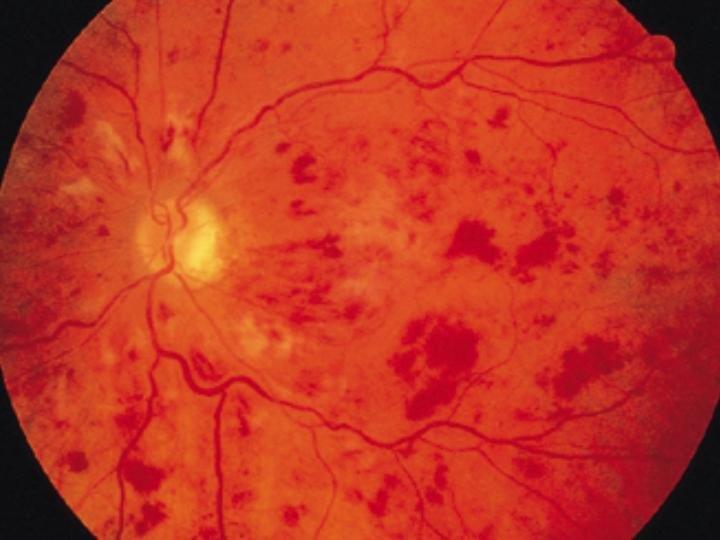
Retinal vascular occlusion significantly affects the vision. The retina is the light-sensitive layer of tissue located on the posterior inner wall of the eyeball. It includes, among other cells, photoreceptors, cones and rodes which receive the light waves and through a complex process this is transferred to the brain where it is converted into an image. It is therefore easy to see that the retina is vital for vision.
The vascular system includes blood vessels called arteries and veins, which carry blood throughout the body, including the eyes. The retina requires continuous blood supply so that its cells receive essential nutrients and oxygen. Also, through the veins, the blood removes “useless” substances, products of retinal metabolism. However, it is possible that one or more of these vessels will be blocked.
Occlusion can cause accumulation of blood or other fluids and thus prevent the retina from properly processing light stimuli. When light is blocked or there is swelling (accumulation of serous fluid), sudden loss of vision may occur. The severity of vision loss may depend on how severe the occlusion is.
Retinal vascular occlusion is a potentially serious condition, especially if atherosclerosis already exists. It occurs most often in middle-aged and elderly people.
Retinal artery occlusion
Occlusion of the main retinal artery is called central retinal artery occlusion. Branch retinal arterial occlusion affects the smaller arteries.
Retinal vein occlusion
Retinal vein occlusion is also divided into two types: central retinal vein (CRVO) occlusion and branch retinal vein occlusion (BRVO)
The blockages of your central vein or artery are usually more severe than branch blockages.
Causes of retinal vascular occlusion.
The exact cause of retinal vascular occlusion is unknown. It can happen when the lumen of the vessels is narrow. However, other factors that affect blood flow increase the risk of developing vascular occlusion.
These factors are:
- atherosclerosis
- blood clots, which “travel” from another area of the body to the eye
- carotid stenosis
- heart disease such as valvular diseases, arrhythmia etc.
- Diabetes
- arterial hypertension
- hyperlipidemia
- obesity
- intravenous drug use
- over 60 years of age
- glaucoma
- smoking
- hematological diseases
- inflammatory disorders such as temporal arteritis
Symptoms of retinal vascular occlusion
The main symptom of retinal vascular occlusion is one-sided, sudden vision disturbance without feeling of pain. This may be related to partial or complete loss of vision. Vision disturbances may be transient or permanent. They require an immediate ophthalmological examination.
Complications of retinal vascular obstruction
- macular edema
- neovascularization (pathological development of blood vessels)
- neovascular glaucoma
- vitreous hemorrhage
Diagnosis of retinal vascular obstruction and extent of damage
- clinical examination
- optical coherence tomography with angiography (OCT-Angiography)
- fluorescein angiography
Investigation of the cause
Control of the cardiovascular system by the cardiologist-internist, blood tests and if necessary further investigation.
Prevention
The best way to prevent retinal vascular occlusion is to identify and treat risk factors. Since retinal vascular occlusion results from systemic vascular problems, it is important to change lifestyles and eating habits to protect the vessels. These changes include:
- exercise
- weight loss if it is an overweighted patient
- healthy diet low in saturated fat
- immediate smoking cessation
- regulation of blood serum sugar levels and blood pressure
Treatment of retinal vascular occlusion
No retinal artery occlusion treatment is available. Most patients experience permanent vision disorder.
Treatment of venous retinal occlusion includes intraocular administration of drugs and sometimes laser therapy. These drugs are the so-called antiangiogenic agents (anti-VEGF) and steroids.

