Retinitis pigmentosa

Retinitis pigmentosa is a category of hereditary diseases in which occurs progressive damage of the photoreceptors and the retinal epithelium pigment layer.
Normal retina Retinitis pigmentosa
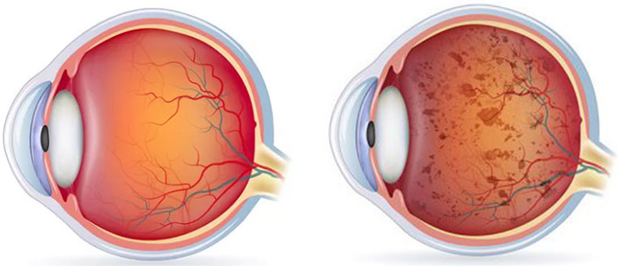
It is usually bilateral, symmetrical, diffuse damage of the photoreceptors, especially the rodes.
In terms of heredity, it can occur sporadically-individually with the dominant, residual autosomal or X-linked character but also as a part of some systemic diseases. Most cases involve sporadic incidents with no known family history. The autosomal dominant character is the next most frequent form, and the X-linked residual character is the least common and the one with the worst prognosis.
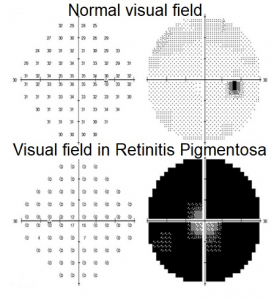
The diagnosis is made through the clinical examination, the photo of autofluorescence of the background of the eye, the examination of the peripheral visual field and the electroretinogram.
More than 3/4 of patients experience nyctalopia at the latest at the age of 30 (inability to adapt to darkness). Gradually occurs a reduction to complete loss of the peripheral visual field but also a decrease in central vision depending on the progression of the disease.
Loss of visual acuity may occur due to macular affection. Approximately 1/4 of patients can read throughout their productive lives despite loss of sight. There are anly a few patients whose visual acuity decreases to levels below 1/10.
Glaucoma, myopia, cystoid macular edema, myopia, hazy vitreous body, drusen of the optic nerve, cataract and keratoconus occur more frequently in patients with retinitis pigmentosa than in the general population.
Normal retinal Retinitis pigmentosa

Treatment of retinitis pigmentosa currently includes procedures to maintain vision (proper nutrition, avoidance of exposure to sunlight, avoidance of smoking, removal of cataract, treatment of cystoid macular edema, treatment of glaucoma, etc.)
Electroretinogram
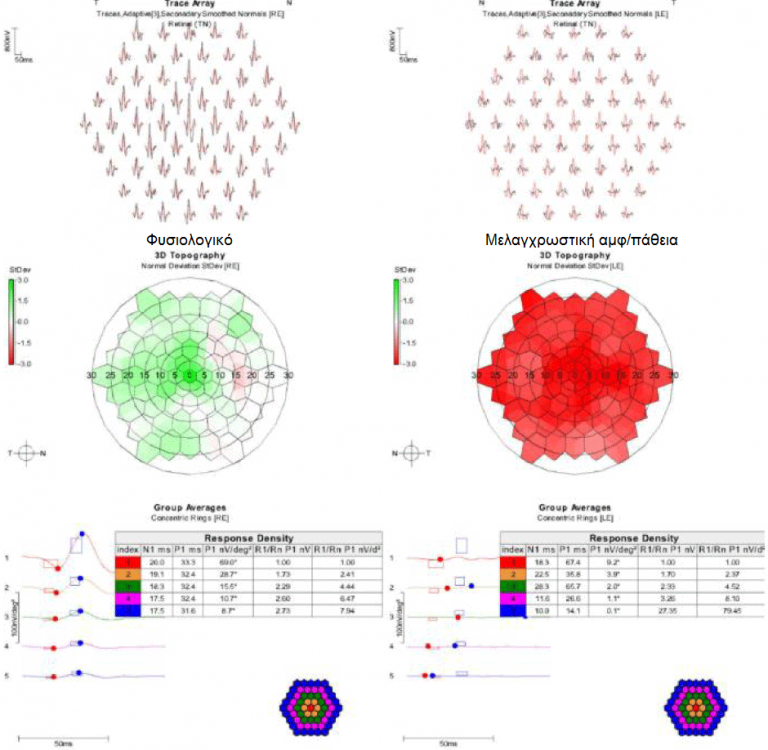
In the last five years, for very advanced forms, and under certain conditions, there is the possibility of gene therapy, which offers not only stabilization but also improvement of vision

