Uveitis

What is uveitis?
Uveitis is usually an inflammation of the middle layer of the eye, which is called uvea. But even inflammations of the retina or sclera and episclera are classified as uveitis; it can be caused by both infectious and non-infectious causes. The uvea consists of the choroid, the ciliary body and the iris.
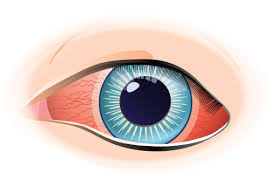
Uveitis is usually not severe. However, the most serious cases can cause even complete, permanent loss of vision if not treated in a timely manner.
Uveitis symptoms?
The following symptoms may occur in one or both eyes:
- severe redness in the eyes
- pain
- dark moving spots in the vision field (floaters)
- sensitivity to light
- blurred vision

What are the causes?
The cause of uveitis is often unknown and often occurs in healthy individuals. Sometimes it is associated with a condition such as an autoimmune disease or infection with a virus or bacterium.
An autoimmune disease occurs when the immune system attacks one or more organs of the body. Some of the autoimmune diseases associated with uveitis are:
- Rheumatoid or other arthritis
- Ankylosing spondylitis
- Psoriasis
- Ulcerative colitis
- Kawasaki Disease
- Crohn’s disease
- Sarcoidosis
- Systemic lupus erythematosus
- Wegener’s disease
- Adamantiadis – Behcet disease
- Multiple sclerosis
Infections are another cause of uveitis.
- AIDS
- Herpes
- Cytomegalovirus (CMV)
- West Nile Virus
- Syphilis
- Toxoplasmosis
- Tuberculosis
- Histoplasmosis
Diagnosis
The diagnosis is initially made through the clinical examination. It is then decided whether it is necessary to refer to a physician specialist in autoimmune diseases as well as blood tests, chest X-ray, MRI etc.
Types of Uveitis
Anterior uveitis
Anterior uveitis is often referred as “iritis” because it attacks the iris. Iritis is the most common type of uveitis and generally occurs in healthy people; it can affect one eye or both at the same time; iritis is usually the least serious type of uveitis.
Middle uveitis (intermediate uveitis )
The middle uveitis affects the middle part of the eye and is also thought to be iridocyclitis. It mainly affects the ciliary body which is the part of the uvea between the iris and the choroid.
Posterior uveitis
Posterior uveitis can also be referred to as choroiditis or retinitis.
Posterior uveitis tends to be the most severe form of uveitis because it can even cause necrosis in the retina or optic nerve. Posterior uveitis is the least common form of uveitis.
Panuveitis
When inflammation affects all the main parts of the eye, it is called panuveitis. It is a combination of findings and symptoms of all three types of uveitis.
How is uveitis treated?
Treatment of uveitis depends on cause and type. In heavier cases, systemic treatment is necessary. If uveitis is the result of systemic disease the treatment is mainly focused on the treatment of the latter. The goal of treatment is to reduce inflammation in the eye.
Here are the common treatment options for each type of uveitis:
- Treatment of anterior uveitis or iritis involves the use of dark glasses, eye drops to dilate the pupil as well as steroid drops.
- Treatment for posterior uveitis may include systemic intake of steroids, injections around the eye and visits to specialists to treat possible underlying infection or autoimmune disease. It is sometimes necessary to systematically take immunosuppressive agents and antibiotics.
- Treatment of middle uveitis includes topical and systemic taking of steroids or other immunosuppressive drugs.
Possible complications from uveitis
- Untreated uveitis can lead to serious complications, such as:
- Cataract
- Permanent corneal blurring
- Macular edema
- Glaucoma
- Retinal detachment
- Atrophy of the optic nerve
Recovery and prognosis
Anterior uveitis usually subsides after a few days of treatment. The posterior is more difficult to treat and usually shows slower recovery. Relapses are not rare. It can last for months to cause permanent vision damage.
How can uveitis be prevented?
Seeking appropriate treatment for autoimmune disease or infection can help prevent uveitis. Uveitis in healthy individuals is difficult to avoid as the cause is not known. Early diagnosis and treatment are important for reducing the risk of vision loss, which can be complete and permanent.

